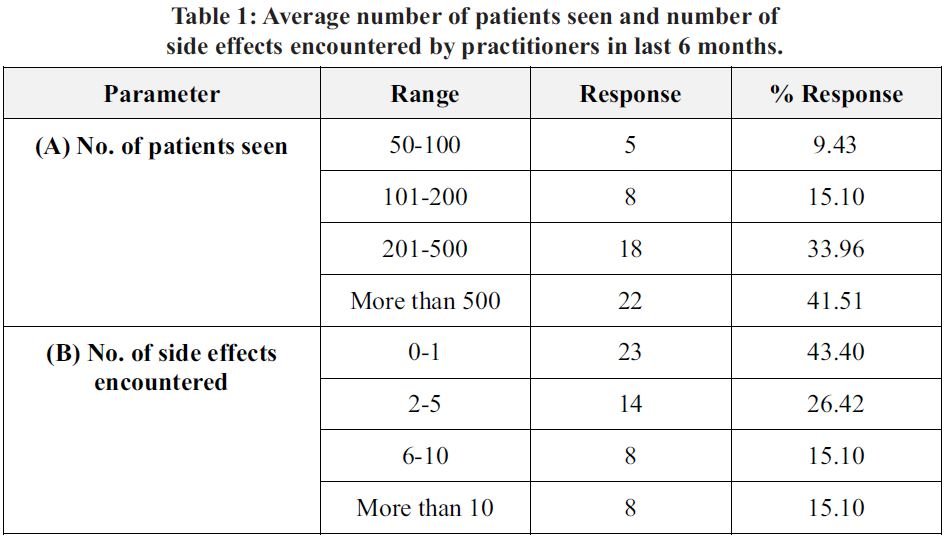
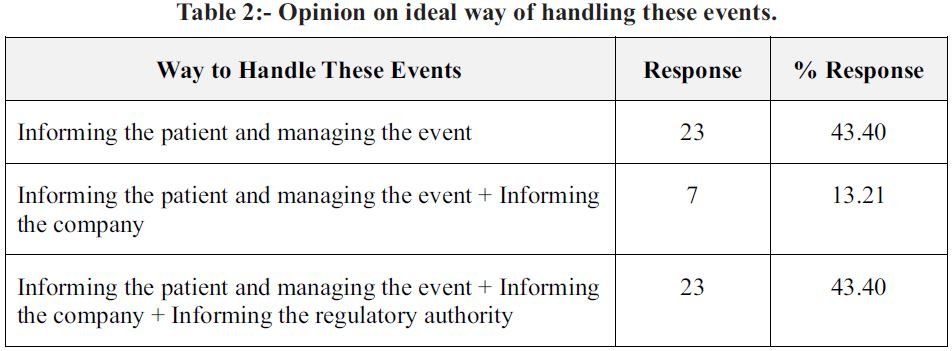
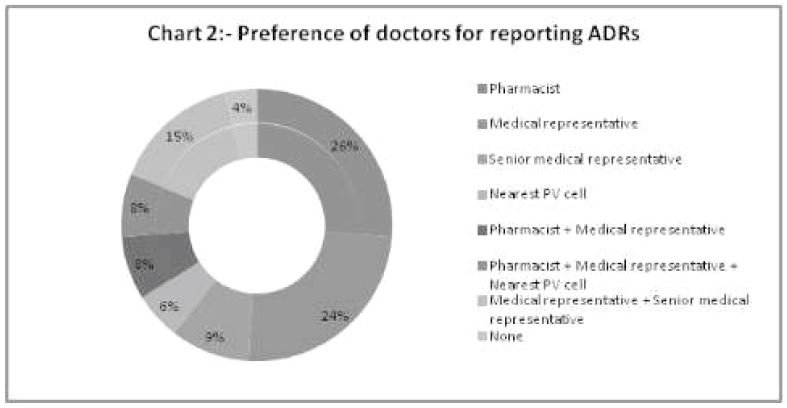
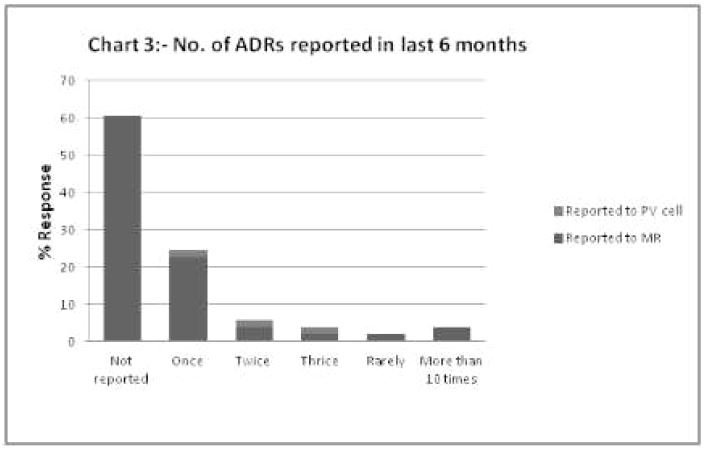
INTRODUCTION
Spontaneous reporting of adverse events (AEs) by the healthcare practitioners, the patient or caregiver is the most widely used and recommended tool to monitor the safety of a marketed medicines. Data form the USFDA lists Adverse drug reactions (ADRs) popularly known as side effects as the 4th leading cause of death in the developed world. Adverse drug reactions (ADRs) not only account for market withdrawals but also for changes in labels or introduction of new-labeled warnings for prescription drugs. (1)
While the drug may have undergone extensive clinical testing during development and its safety profile largely known, the very nature of it being done on a limited number of patients in controlled trial conditions precludes many of the rare AEs being detected. Once marketed,